Pediatrics is the branch of medicine that deals with the prevention and treatment of children, as well as counseling with parents.
Preventive Pediatrics deals with healthy children and includes:
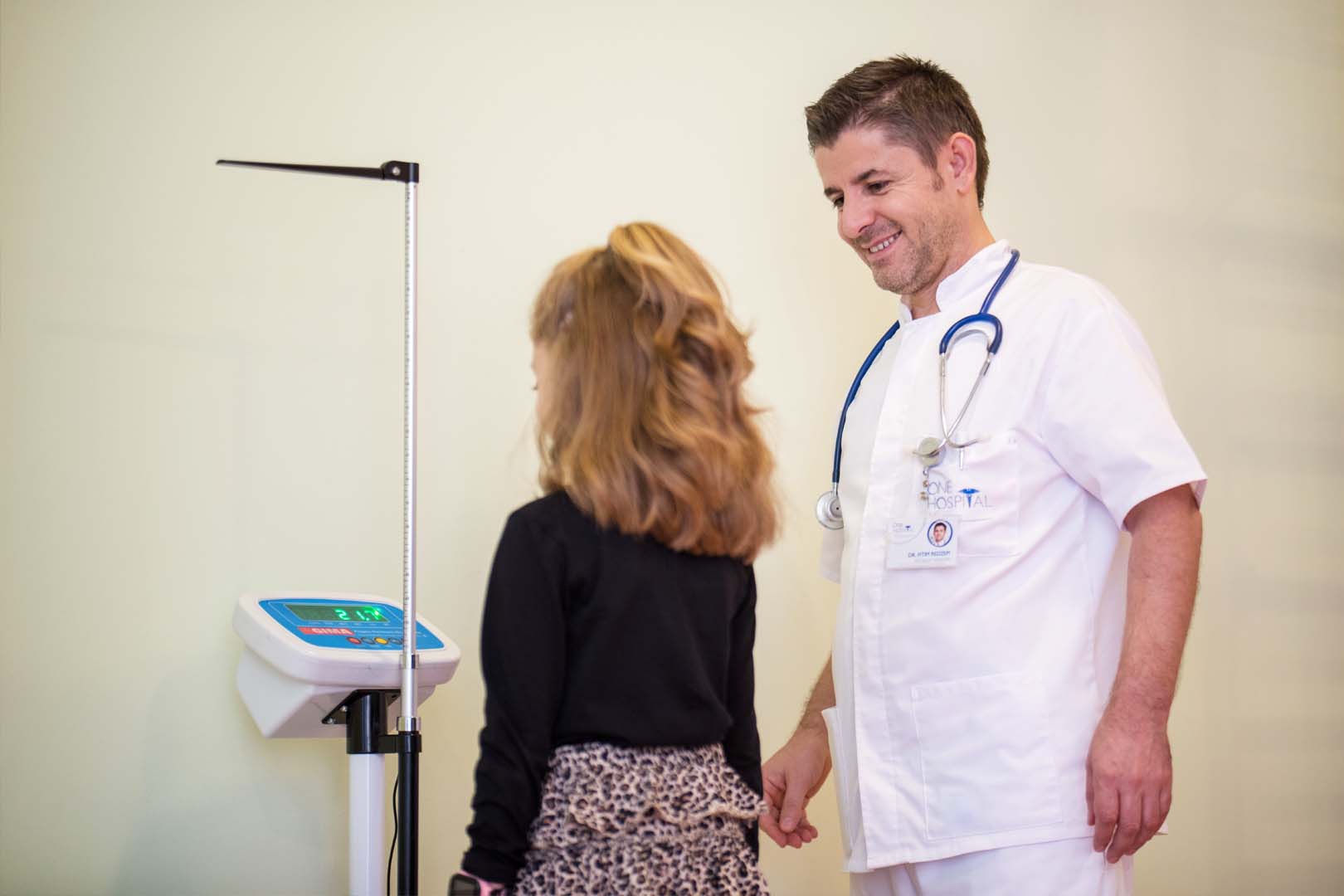
Monitoring the growth and development of the child
Vaccination according to national and international vaccination calendars
Ultrasound imaging of the hips in the first year of life
Systematic examinations for preschool and after school
Taking care of the health and treatment of children is also a preventive remedy for the adult population. Taking care of the children aims to prevent illnesses by vaccinating and regular screening of children of all ages.
The systematic (preventive) examinations are the basis for regular monitoring of a child’s health and vary with age.
Systematic examination includes weight measurement, head circumference, chest, and examination of all the senses, heart, lungs, bones and muscles. This allows growth and development monitoring, signs of puberty, spinal condition, weight gain, bad eating habits and daily lifestyle, as well as timely detection of diseases and disorders.
In the treatment and follow-up of chronically ill children, education about new lifestyles and treatment is inevitable, which alleviates the severity and course of chronic illness, but also greatly improves the quality of life of a chronically ill child.
If you have any questions, please contact us at: [email protected] or +389 (0) 44 344 414
To schedule an examination, click here
If you have any questions, please contact us at: [email protected] or +389 (0) 44 344 414
To schedule an examination, click here
Categories
Respiratory infections are the most common infections in the pediatric age and are divided into upper and lower respiratory infections. Upper respiratory infections are more prevalent and most commonly in pediatrics. The most common of these are viruses, but to a lesser extent we can also have bacterial or atypical infections. Lower respiratory infections, more serious than the above, are being given more attention by parents and also by us pediatricians, and should be treated in appropriate settings.
These infections also include allergic reactions from aeroallergens that require appropriate prevention and treatment.
Urinary tract infections after upper respiratory tract infections are one of the most common infections in children. Urinary tract infections are divided into upper urinary tract infections and lower urinary tract infections. Lower urinary tract infections the most common cause of urinary tract infections are bacteria and E. coli is more common in smaller scales and chlamydia or proteus.
Symptoms are different and these symptoms manifest differently depending on the age of the children. The upper infections are more difficult to copy and the clinical picture is more pronounced with elevated temperature, vomiting, abdominal discomfort, rejection of the diet with infants, atypical symptomatology such as jaundice, anxiety, vomiting, non-progression in weight, convulsions, etc.
Lower bladder infections, or bladder infections, are milder symptomatology and do not give rise to vomiting or fever, but we do have an abdominal discomfort where children are restless complaining of suprapubic region with dysuria, frequency or establishing order and rhythm of urinary control are beginning to lose this control.
What should we do?
Pediatric control of a child, a general examination is carried out by taking blood and urine to see if we have elevated leukocytes as well as urine to detect leukocytes, bacteria and nitrites. If we have elevated leukocytes in the bloodstream, we have high values. CRP (inflammation indicator) as well as leukocytes in the urine above 10 High Power Field leukocytes then should be considered pyelonephritis or kidney infection and should be treated with antibiotics. While if we only have elevated leukocytes only in urine and calm leukocytes in blood and milder symptoms then it is a bladder infection or infection of the lower urinary tract and is treated with antibiotics per os (orally).
Anemia is a decrease in hemoglobin values and a decrease in the number of red blood cells in the blood. Anemia in children is common especially after 5-6 months due to iron deficiency and increased growth and development of a child at that age when needs iron.
Usually children have pale skin and mucous membranes, irritability, decreased appetite, general weakness, etc. Analyzes provide a blood count of the hemoglobin and other parameters such as hematocrit, MCV, and iron in the blood.
Therapy – If we have low levels of hemoglobin, a therapeutic dose of iron is given according to the child’s weight. But it is also given in preventive doses of iron in cases of borderline anemia in a child of growth and development age.
Jaundice or icterus is high levels of bilirubin in the blood. Bilirubin is divided into direct and indirect bilirubin.
Infantile jaundice after the second day of birth up to 2 weeks is a physiological jaundice and in most cases is of an indirect type.
The most important thing is that the jaundice occurs after the second day of birth and does not persist for more than 2 weeks. In cases where the jaundice occurs since day one or persists for more than 2 weeks and is feverish, sleepy, organomegaly and other symptoms the infant should be referred to a pediatrician and laboratory tests starting with Bilirubin, direct and indirect, should be performed imaging, hemp, urine sedimentation and other laboratory investigations to determine the etiology of prolonged or high blood bilirubin value.




